· pain-guides · 6 min read
Chest Pain Causes: 5 Reasons Your Chest Hurts and When to Worry
Chest pain is scary, but it isn't always your heart. Learn the most common chest pain causes — from muscle strain to acid reflux — and how a simple pain map can help you communicate more clearly with your doctor.
You feel a tightness in your chest, maybe a dull ache or a sharp twinge that catches you off guard. Your mind immediately goes to the worst-case scenario. But here’s the thing — most chest pain isn’t a heart attack. In fact, musculoskeletal issues, acid reflux, and stress account for the vast majority of chest pain cases that walk through a doctor’s door.
That doesn’t mean you should ignore it. But understanding what’s behind that discomfort can save you a lot of anxiety — and help you communicate more clearly with your doctor when it matters.
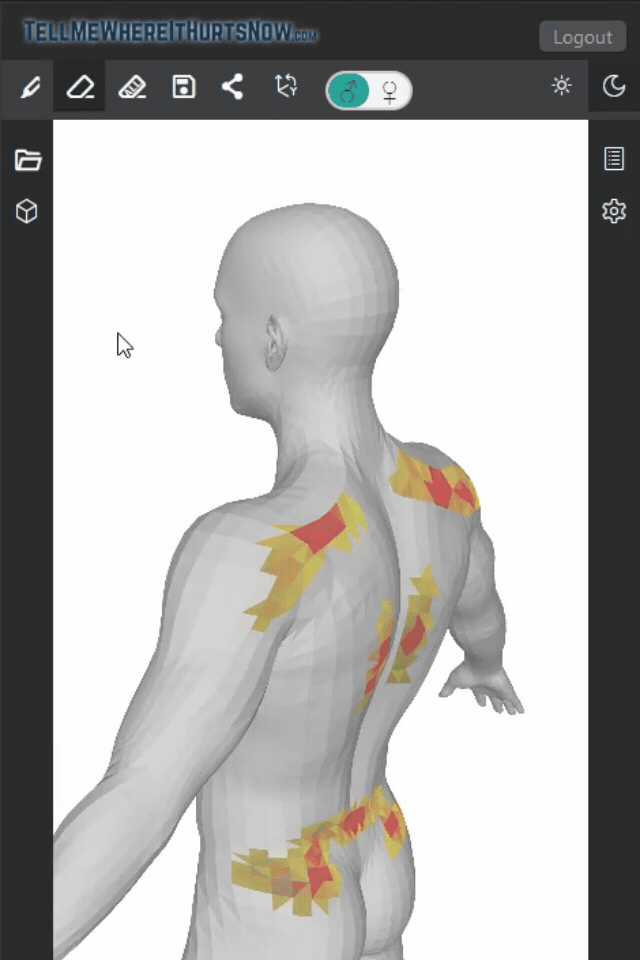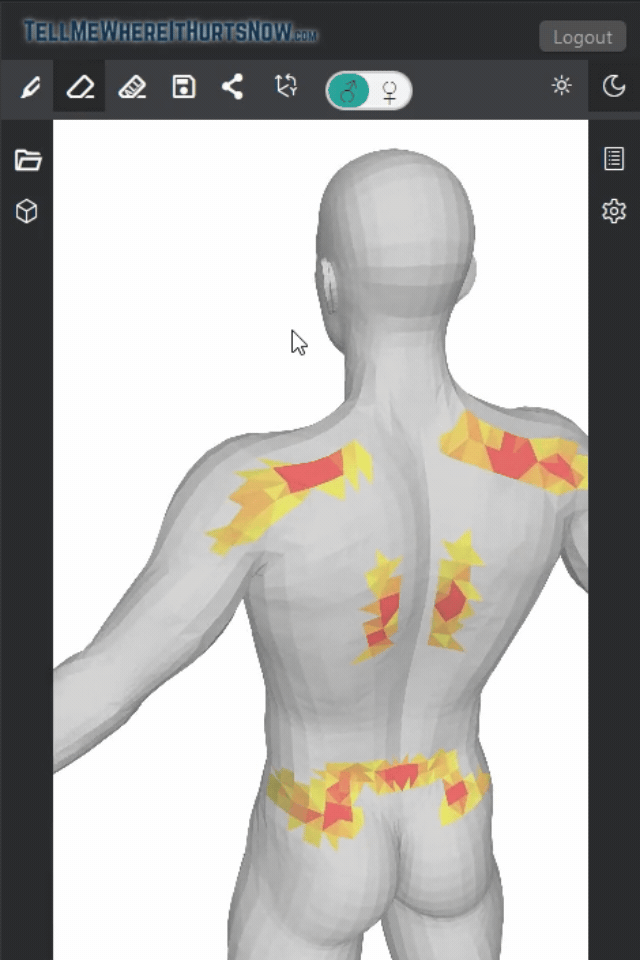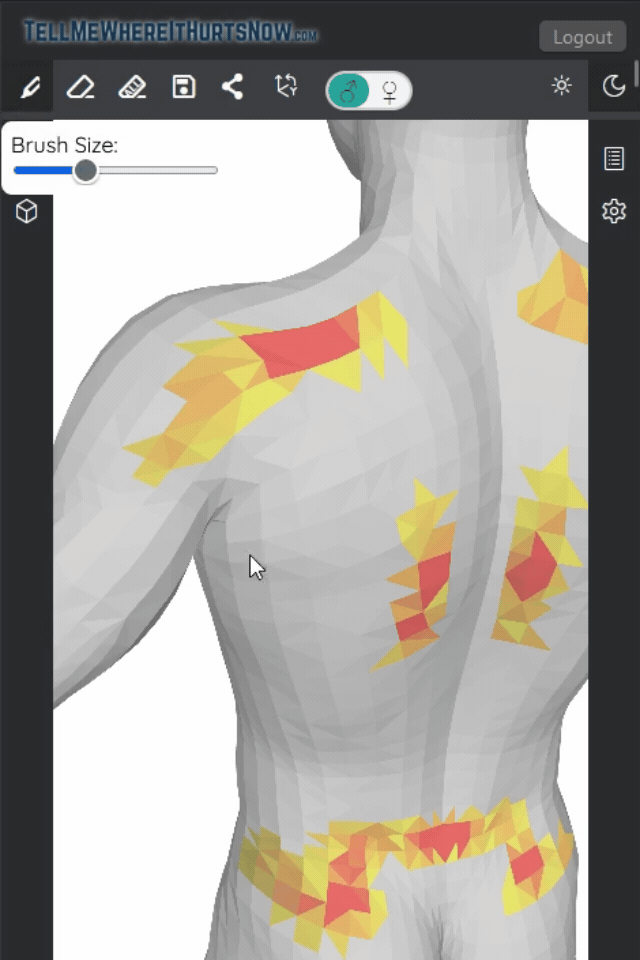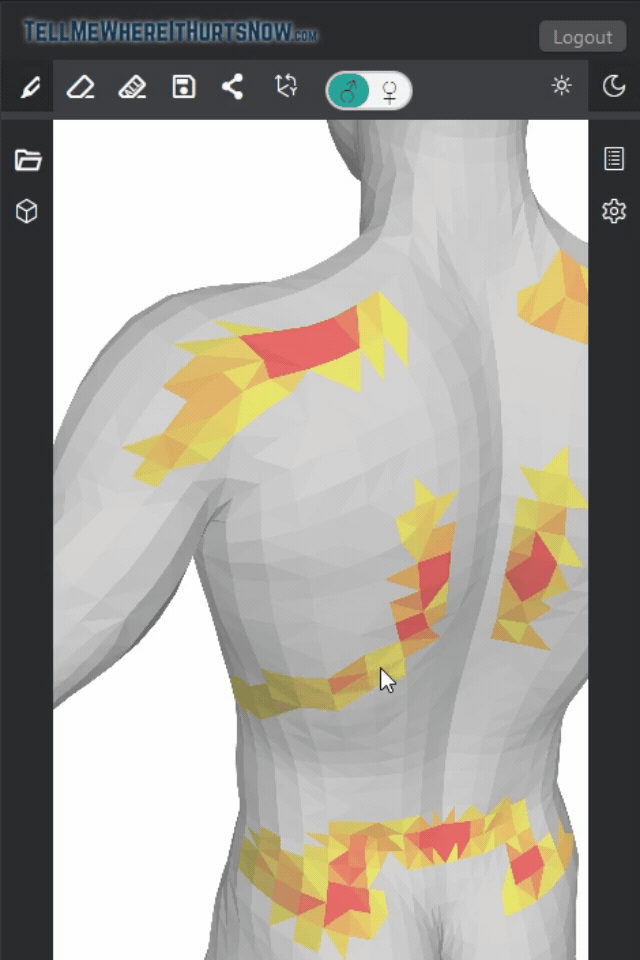
We recently analyzed pain maps from 22 patients over the past week using TellMeWhereItHurtsNow.com, and chest and pectoral pain was the single most reported area, showing up in nearly half of all maps. It’s clearly something a lot of people are dealing with.
Know exactly where your pain is? Show your doctor. Patients who use visual pain maps get faster, more accurate diagnoses. See how it works →
What Causes Chest Pain That Isn’t a Heart Attack?
This is probably the first question that pops into your head when your chest starts hurting. The good news is that there are several common, non-cardiac explanations.
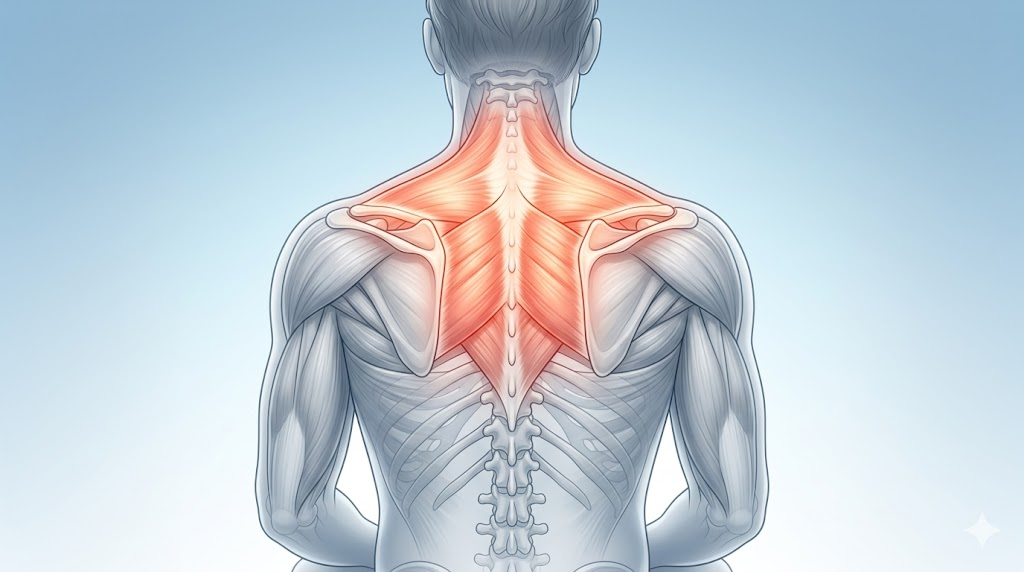
Musculoskeletal strain is one of the most frequent culprits. If you’ve been working out, lifting something heavy, or even coughing a lot recently, the muscles between your ribs (called intercostal muscles) can get irritated or strained. This type of pain usually feels sharp and gets worse when you move, twist, or take a deep breath. It often responds well to rest and over-the-counter anti-inflammatories like ibuprofen.
Costochondritis is another common cause — it’s inflammation of the cartilage that connects your ribs to your breastbone. It can feel alarming because the pain is right in the center of your chest, but it’s typically harmless and resolves on its own within a few weeks.
Acid reflux (GERD) can also mimic chest pain so convincingly that many people end up in the emergency room thinking they’re having a heart attack. The burning sensation from stomach acid backing up into your esophagus can radiate across your chest, especially after eating or when lying down.
How Do I Know If My Chest Pain Is Muscular?
Muscular chest pain has some telltale signs that set it apart from cardiac pain. Here’s what to look for:
- It’s reproducible. If you can press on the sore spot and make the pain worse, it’s likely musculoskeletal. Heart pain doesn’t respond to touch.
- It changes with movement. If twisting your torso, reaching overhead, or taking a deep breath makes it worse, that points to muscles or ribs rather than your heart.
- You can pinpoint it. Muscular pain tends to be localized — you can point to exactly where it hurts. Cardiac pain is more diffuse, often described as pressure or squeezing across the whole chest.
- It came after physical activity. If you hit the gym, moved furniture, or did yard work before the pain started, muscle strain is the most likely explanation.
In our pain mapping data, we noticed that male users tend to show intense, focal red spots on their chest — consistent with localized muscle strain. Female users, on the other hand, often show broader, more diffuse highlighting across the chest and shoulders, which could indicate a different pattern of musculoskeletal involvement.
Not sure how to describe your pain to your doctor? Map it visually in 60 seconds →
When Should I Worry About Chest Pain?
While most chest pain is benign, some situations warrant immediate medical attention. Call 911 or go to the emergency room if:
- The pain is sudden and severe, especially if it feels like pressure, squeezing, or a heavy weight on your chest
- It radiates to your arm, jaw, neck, or back
- You also have shortness of breath, nausea, lightheadedness, or cold sweats
- It doesn’t go away after 5 minutes of rest
- You have risk factors like a history of heart disease, high blood pressure, diabetes, smoking, or a family history of heart attacks
The key distinction is pattern. Muscular pain is usually sharp and localized. Cardiac pain is usually described as pressure or tightness that’s hard to pinpoint. If you’re ever unsure, err on the side of caution — it’s always better to get checked and find out it’s nothing than to ignore something serious.
Could Stress or Anxiety Be Causing My Chest Pain?
Absolutely. Anxiety-related chest pain is more common than most people realize, and it can feel genuinely frightening. During a panic attack or period of high stress, your body’s fight-or-flight response kicks in, causing your muscles to tense up (including those in your chest), your heart rate to increase, and your breathing to become shallow.
This combination can produce chest tightness, sharp pains, and even a feeling of not being able to catch your breath — symptoms that closely mimic a heart attack. The pain is real, even though the cause isn’t cardiac.
If you notice that your chest pain tends to show up during stressful periods, comes with racing thoughts or a sense of dread, and goes away once you calm down, anxiety might be the driver. Deep breathing exercises, regular physical activity, and working with a therapist can all help manage stress-related chest pain.
What You Can Do About It
If your chest pain isn’t an emergency, there are several practical steps you can take:
- For muscle strain: Rest the area, apply a warm compress, and take ibuprofen or acetaminophen. Gentle stretching of the pectoral and intercostal muscles can help once the acute pain subsides.
- For acid reflux: Avoid eating within 2-3 hours of lying down. Cut back on spicy, fatty, or acidic foods. Over-the-counter antacids or proton pump inhibitors can help.
- For stress-related pain: Practice deep breathing — inhale for 4 counts, hold for 4, exhale for 4. Regular exercise, adequate sleep, and reducing caffeine can also help.
- For costochondritis: Apply heat to the affected area and avoid activities that aggravate the pain. It usually resolves in a few weeks.
- Track your pain over time — use TellMeWhereItHurtsNow.com to log where it hurts, how intense it is, and how it changes. Export the report to share with your doctor.
See Exactly Where Your Chest Pain Is (And Share It With Your Doctor)
One of the hardest parts of dealing with chest pain is explaining it to your doctor. Saying “my chest hurts” doesn’t capture where exactly it hurts, how intense it is, or how it’s changed since your last visit.
Stop struggling to describe your chest pain. With TellMeWhereItHurtsNow.com, you can mark exactly where your chest pain is on a 3D body model, rate its intensity with a color-coded scale, and share the result directly with your doctor — giving them a clear picture in seconds instead of a vague description. Free to try, no signup required.